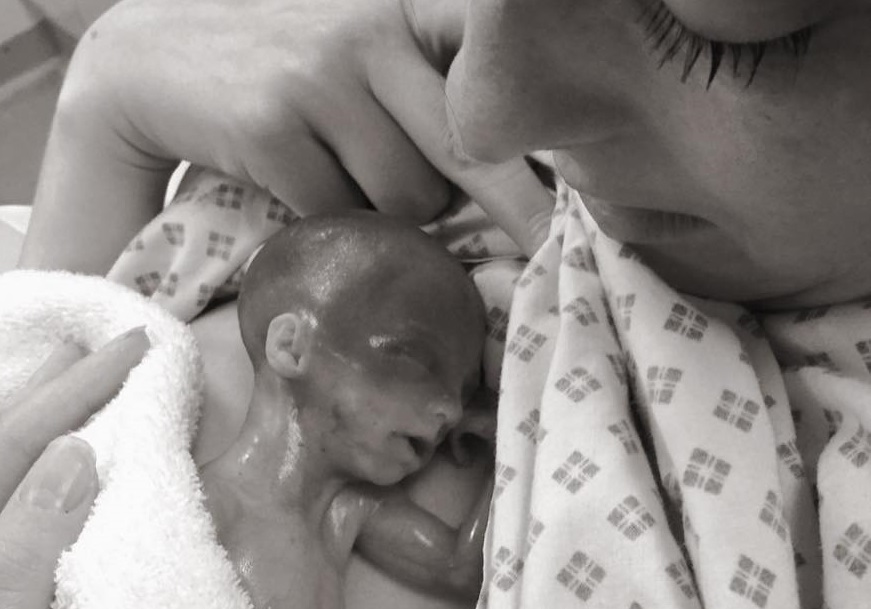
Unexpectedly pregnant with their sixth child, Sophie Dennis and her husband were initially shocked, but by the time they traveled from the United Kingdom to Spain for their family vacation at 13 weeks gestation, they loved their new preborn child as much as any of their others. However, that vacation would be the beginning of a heartbreaking struggle to save their preborn baby girl only to tragically lose her, they say, due to medical negligence. Baby Autumn would be born extremely premature at 22 weeks and six days gestation – a gray area in which some doctors would offer her medical intervention, but others would not. Autumn’s doctors would choose the latter, despite her mother Sophie’s repeated requests for help for her premature baby. Some children born as early as 21 weeks have survived, thanks to medical assistance.
While on vacation, Sophie began to experience bleeding so heavy that she had to wrap a towel around herself. She went to the local hospital, but a language barrier kept her from fully understanding what was happening. Thankfully, the woman they were renting their vacation apartment from accompanied her and was able to explain some of what the doctors were saying.
“I just remember them saying the word hematoma and the measurements of it,” Sophie told Live Action News. “So the two weeks spent there I did a lot of googling. Subchronic hematoma 3.2 cm. I phoned home a few times to speak to someone at the hospital. I’m sensitive. I’m obviously worried. The bleeding started again and I bleed for the rest of the holiday. But it wasn’t fresh blood so that was good.”

Premature baby girl Autumn and her parents (Facebook)
As soon as they arrived back in the United Kingdom, Sophie went to the hospital where an ultrasound revealed baby Autumn was perfectly content – a huge relief. Sophie’s cervix was closed as well, which was another good sign. However, doctors did not check the size of the hematoma and instead scheduled a scan for two weeks later to measure it. Sophie expressed her dissatisfaction, but there was nothing she could do. She went home, happy that her daughter was safe, and researched outcomes of pregnancies with hematoma.
When she returned for the scan to measure the hematoma, doctors told her that most of the time the body simply reabsorbs it or it continues to grow. They assured her that women go on to have healthy pregnancies and that while she could go into preterm labor, in her case, she was most likely to have miscarried the baby while she was on vacation. The hematoma had grown from 3.2 to 7.2 cm.
“The told me, ‘The baby looks good, and there was no fresh bleeding’,” said Sophie. “But blood is an irritant to the uterus so that can cause contractions. It should have been a warning sign to keep an eye on this lady and this baby.”
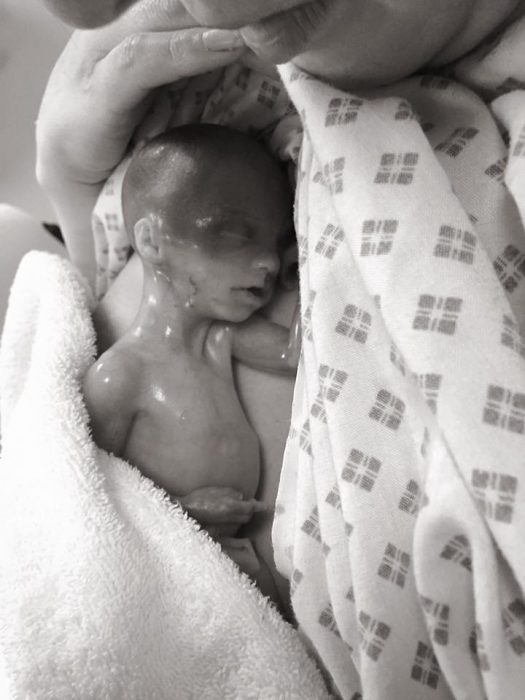
Premature baby girl Autumn (Facebook)
Sophie was told they would continue to monitor her by performing a scan every couple of weeks; however, those frequent scans never happened and doctors told her there was nothing that could be done to prevent preterm labor and that there would be no benefit to the scans. But Sophie had researched steps to take, such as not walking far distances, no heavy lifting, and no sex. The doctors advised her that these things wouldn’t make much difference and that she needed to make it to 24 weeks gestation, otherwise they wouldn’t take any steps to save her daughter.
“They told me to come back at 20 weeks. I was shocked,” said Sophie. “I’ve got a blood clot in my uterus. It’s moved. It’s grown in size. I was getting headaches and feeling unwell. And he thought ‘Just a normal pregnancy’. I have one kidney and I’m prone to water [UTI] infections. We came back at 20 weeks and the blood clot was from the cervix to the uterine wall. I had stopped bleeding for a few days and the baby looked good, all looked good. We saw the same guy again and we were literally in and out in five minutes and he said the same as he said before: ‘If you had any pain and fresh bleeding come straight in.’ Me being unwell, which was on and off for a few weeks, I put it off to catching what the kids had. Pain I had I put all that down to round ligament pain and general pregnancy. I didn’t really know what I was looking for besides blood clot and bleeding. They never told me whether or not I had a water infection. He told me to come back in six weeks. I said that’s ridiculous, I thought you were going to scan me regular.”
The doctor said it was out of his hands and told Sophie, “You do what you feel like you need to do.” Sophie felt no one was as concerned as she thought they should be and though the bleeding had at least momentarily stopped, she left the hospital feeling even more worried about her baby and completely unsupported.
Then, at 22 weeks and five days gestation, Sophie went into preterm labor. As she sat in the waiting room at the hospital, watching as another mother was wheeled in before her, she broke down in tears. After the midwives and doctors finally came to help her, they said the baby was doing fine, but that labor couldn’t be stopped and the baby girl would be born that night.
“The midwife said, ‘I’m sorry, there’s nothing we can do. Your membranes are in the birth canal; she’s coming tonight’. I remember letting out this cry. I’m pretty sure the whole hospital heard me,” said Sophie.
READ: Miracle: Born at 21 weeks, ‘most premature’ baby is thriving
Sophie asked if they could help her daughter, but the doctors said at this age there was nothing to be done. They said that if she did survive because of medical intervention she ran the risk of being disabled. And though Sophie argued that other babies born at 22 weeks had survived and thrived, the doctor told her not to believe what she read on the internet.
Feeling patronized and knowing that other hospitals in the country had helped children born at 23 weeks, Sophie was in shock that the doctors were refusing to help her daughter at 22 weeks and six days. As she was wheeled into a labor room, she again asked them to help her baby. Again doctors told her she would be “poorly and disabled” if she lived. Sophie hoped that if her daughter were breathing at birth that the doctors would step in.
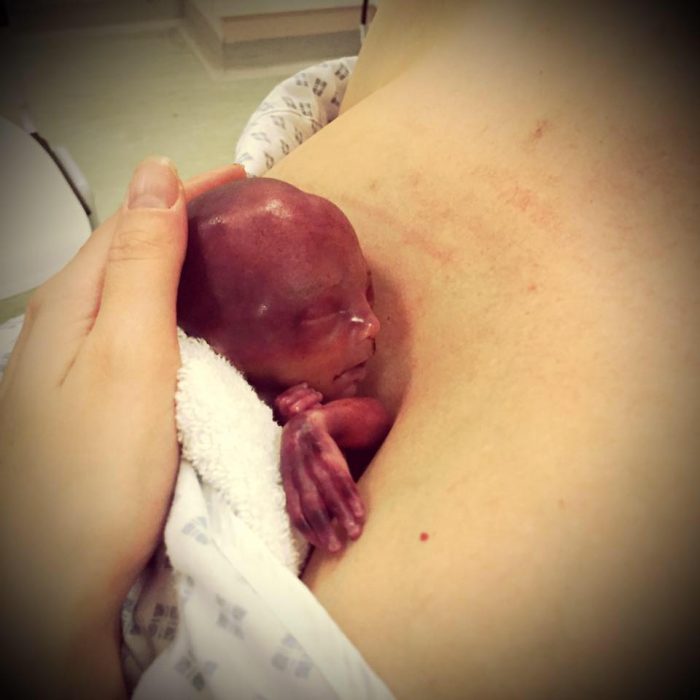
Premature baby girl Autumn. Facebook.
In the early morning hours, at 22 weeks and six days gestation, Autumn Orion was born breathing. However, that help Sophie so desperately wanted never came.
“I remember I didn’t want to push and I’m crying and screaming and praying to God to help my child,” recalled Sophie. “They placed her on me. She’s there and I remember very clearly her moving her arms and legs. […] She was gasping for air. She did at least six big gasps. She needed help. She needed them to help her and they did nothing.”
Autumn lived for nearly two hours outside the womb. Her parents continued to question the medical team about helping her.
After Autumn’s funeral, Sophie and her husband met with a neonatologist whom they questioned further about why their daughter wasn’t helped. According to Sophie, all of the information the doctor used to justify not helping Autumn was misinformation. He argued that she didn’t weigh enough, but Sophie said they didn’t weigh her immediately after birth. He argued that her heart rate was only 60 beats per minute, but Sophie said they didn’t check her heartbeat until well after her birth.
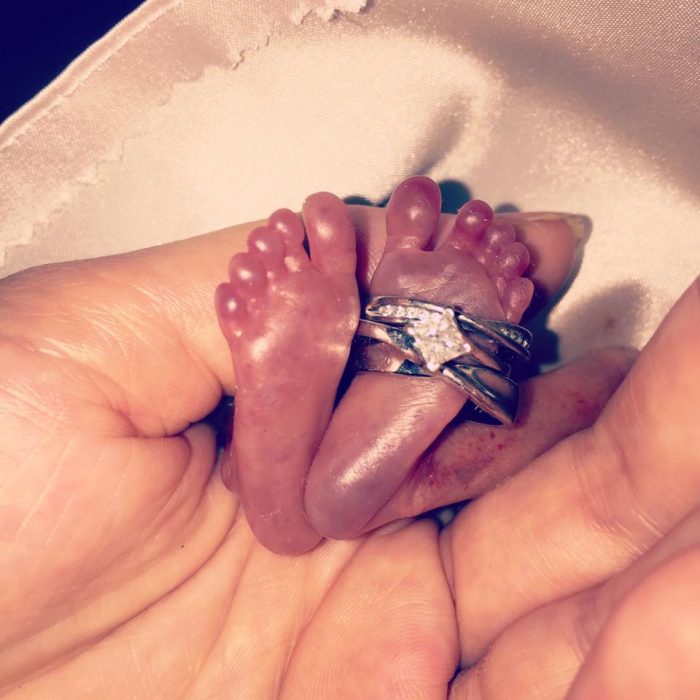
Premature baby girl Autumn’s tiny feet with her parents’ wedding bands (Facebook)
“I remember shouting at this doctor. He said her heart was 60 beats per minute, but they never took her heart rate. They were going on about her weight but they didn’t weigh her at birth. You can’t tell me she didn’t weigh enough. You can’t be certain that she wouldn’t have lived if you helped her. They’re moving the goalpost,” said Sophie. “You didn’t give her the option and it was taken away from her. You tell me now, look at me in the eyes and tell me now if I had asked you to do everything that you would have helped my baby.”
The doctor admitted that if he were the doctor delivering Autumn and Sophie had pushed him enough, he would have tried to save her.
“I told him, ‘You massively, massively let me and my child down. You should be telling the parents this information and you do save babies in the gray area. If you had helped her you don’t know how that baby would have responded. You’re not God and you’re not a crystal ball. The fact that you didn’t try that makes it different. If she did pass I could look you in the eye and say thank you for trying. You decided her fate, not God, and now I’ve got to live with that forever. It can’t happen again. It just can’t,” said Sophie.

Premature baby girl Autumn and her mother. Facebook.
Sophie and her husband have been following the story of baby Benson, a premature baby born at 22 weeks five days gestation. Doctors stepped in to help Benson, and today, he is doing well. She wishes she could say the same for Autumn, and cries because she feels if doctors had stepped in, Benson’s story could have also been Autumn’s.
“I’ve got to live for the rest of my life knowing that there was more I could have done and that was taken away from me because of people not doing their job properly,” she said. “I’ve got to live the rest of my life knowing that my baby girl died on me, fighting to breathe. She suffocated to death.”
Sophie is working with a lawyer and has started a petition so that no other mother has to suffer this way again. She wants any child born at 22 weeks to be helped and she wants the parents to be able to make that call, not the doctors.
“It should be normal [to help babies]. It should be fluent between hospitals,” said Sophie. “This is the NHS. The guidelines are supposed to be… the same. If we had been somewhere else they could have done something. They let me down in my pregnancy and they let me down when I had her and I don’t want that happen to another mom. I promised Autumn I would try to do everything I could to change things.”