The name Israel means he who prevails with God. Right now, there is an emergency calling for the performance of God’s love and work here on earth. In no uncertain terms, prevailing in this instance means life and losing results in death.
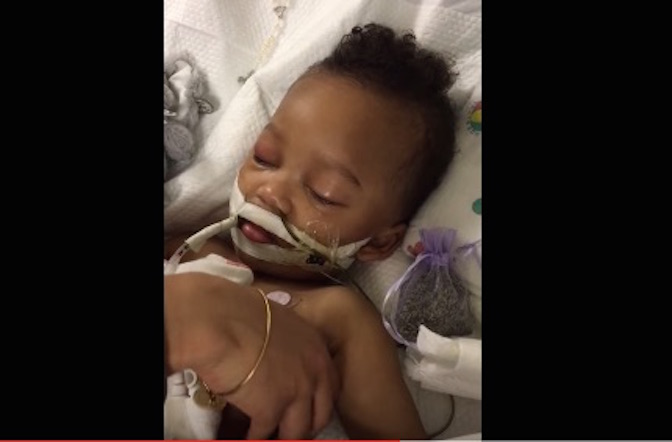
Israel Stinson is a beautiful two-year-old boy with baby soft caramel skin and big brown sparkling eyes, the kind that penetrate through your chest and make you feel as if part of your heart is smiling. Israel’s mom uses her graceful fingers to comb Israel’s dark curls into a pile on the top of his head that gently rests on a white pillow case at the Kaiser Permanente Medical Center in Roseville, California—the hospital determined to end Israel Stinson’s young life.
Yesterday, the parents of two-year-old Israel Stinson took the next steps in their battle to stop the hospital, currently housing their son, from carrying out its decision to end Israel’s life. Israel’s parents, with the help of their heroic attorneys from the Life Legal Defense Foundation, asked Judge Kimberly Mueller to restrain the hospital from unplugging Israel’s ventilator, a move, that the hospital knows, will kill two-year-old Israel by suffocation.
Just one month ago on April 1st, Israel’s parents could not have imagined this fate. It was the week after Easter Sunday. Israel was running around like a normal, active two-year old. Israel was enjoying his role of responsible and loving older brother to his younger sister. Israel was laughing, sharing his contagious grin, and beaming with life and innocence. But then the protective shield a mother builds around her child was pierced as Israel’s mom found herself rushing to an emergency room. Israel was having trouble breathing, fighting an asthma attack.
The physicians in the emergency room placed Israel on a breathing machine and took x-rays. Eventually, the physicians intubated Israel and transferred him to a different hospital with a pediatric unit. There, on the very next day, Israel’s tube was removed. The hospital declared Israel was stable and told Israel’s parents that they could probably go home the following day. This never happened.
About an hour and a half later, the relief of this news drained from the room as Israel began wheezing and gasping to breathe again. Instead of providing a breathing tube, physicians attempted other methods that proved unsuccessful. Israel’s body went limp, and the hospital eventually performed CPR to resuscitate Israel’s tiny body. Doctors placed Israel on life support but encouraged Israel’s parents that he was “going to make it.” Later, doctors shared that a possibility of brain damage existed due the lack of oxygen to Israel’s brain prior to connecting Israel to life support.
Three days later, on April 6th, doctors determined that Israel’s heart and lungs were functioning on their own. Then six days after that, doctors transferred Israel to yet another hospital, the Kaiser Permanente Medical Center. It is here, within 24 hours of receiving Israel, that the hospital told Israel’s parents that they would likely withdraw life support. Indeed, just two days after being transferred to Kaiser Permanente Medical Center, the hospital pronounced two-year Israel “brain dead.”
To the hospital, this pronouncement means that Israel’s parents no longer have the right to exercise any decision making authority regarding Israel’s placement on a ventilator. Simply put, the hospital can unplug the machine that is keeping Israel alive. Israel’s parents filed a petition with the state court, begging the court to order the hospital to continue treatment and give their son more time. The state court temporarily restrained the hospital from removing the ventilator for the family to make arrangements for their son to be transferred to another hospital.
Dr. Paul Byrne, a board certified neonatologist, pediatrician, and Clinical Professor, visited Israel and examined his medical records. Dr. Paul Byrne wants everyone to know: “Israel is alive.”
Dr. Paul Byrne is an expert in traumatic brain injury, like Israel’s. In 1975, Dr. Paul Byrne treated a young man that some physicians concluded was brain dead and was on a ventilator for 6 weeks. The young man eventually gained full consciousness and was weaned from the ventilator. The man went on to live a full life, is married, and has three children. Dr. Paul Byrne also treated Jahi McMath, whose parents also had to take hospital administrators to court in order to save the life of their child. Since being declared “brain dead,” Jahi has celebrated her 14th and 15th birthdays, and is constantly surrounded by the love of her family.
Dr. Paul Byrne discovered that the hospital was failing to give Israel the nutrients and treatments he needed to recover. The hospital refused to change their treatment at the request of Israel’s parents claiming that “they do not treat or feed brain dead patients” and that Israel’s parents no longer have the ability to make decisions over their son’s healthcare.
In the past week, Israel has shown improvement. Israel’s heart continues to beat on its own. Israel responds to his mother’s voice, took breaths on his own, and even lifted his arm. The hospital, however, refuses to back down and is fighting to remove Israel’s life support.
Israel’s family and legal counsel find themselves in a race against time. Unable to secure placement in a different facility before the expiration of the state court’s temporary restraining order, the family filed an emergency motion with the federal court last Friday to stop the hospital from ending Israel’s life and to obtain more time. Yesterday, the federal court restrained the hospital from removing life support until May 11th, giving Israel’s family a brief reprieve. The family hopes that May 11th does not come too soon.
Israel currently needs a hospital willing to accept him and a doctor who is board certified in California to perform a tracheotomy and insert a feeding tube for Israel to breathe and receive nutrients while in transport to a new hospital. Perhaps someone in a position to help might read this article and rise to the challenge of helping Israel.
Critics may say recovery is impossible. That Israel’s parents should just give up. But why should Israel’s parents be forced into blind obeisance to a hospital, especially when there are conflicting opinions about their son’s condition? And, above all, when doing so will result in the death of their beautiful, two-year old son? Both Israel’s legal challenges against the hospital and his physical recovery pose significant, seemingly insurmountable, battles. But maybe there are times in life when love and the will to live can decimate the impossible to nothing. And maybe the truly wise know that nothing—absolutely nothing—is impossible for God.